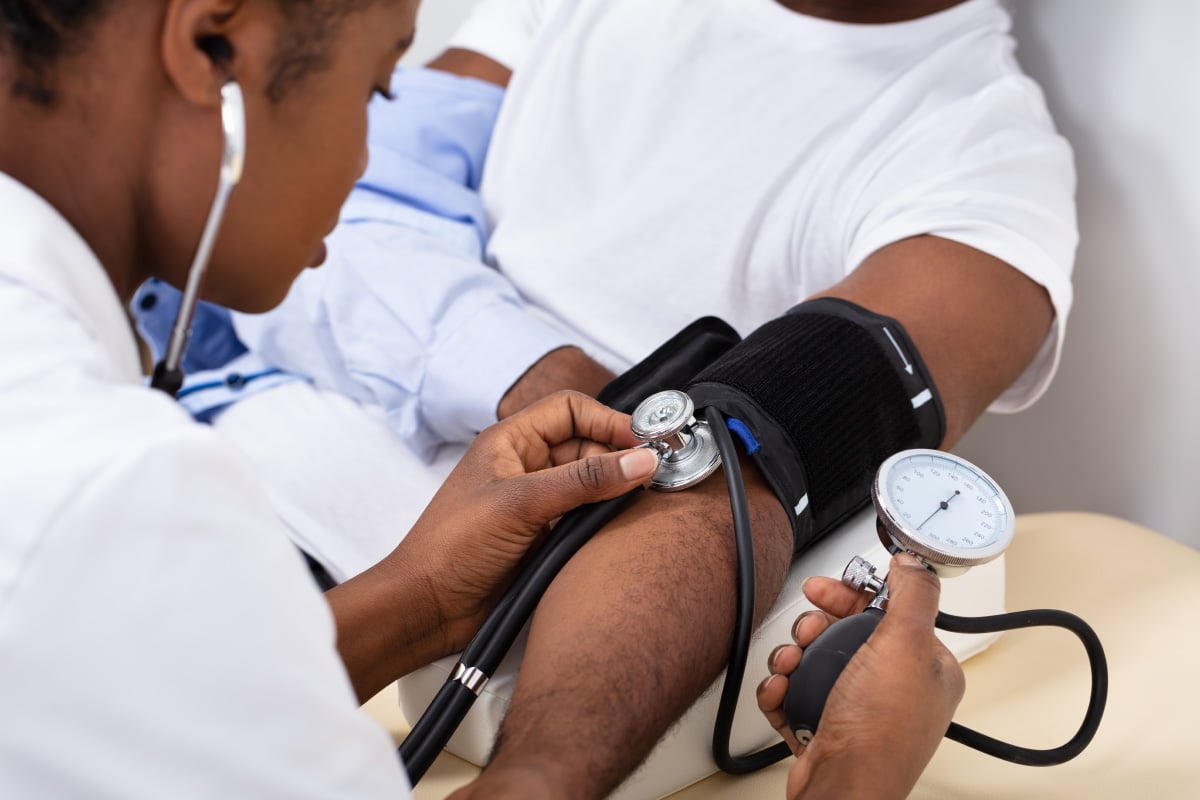
Three Ways to Make Safer Decisions when Selecting Substitute Products in Nonacute Care
Healthcare providers continue to face widespread economic challenges that directly affect the supply chain—from record inflation and dwindling margins, to shortages of supplies and workers, to cost increases in labor and supplies. In a survey conducted by Kaufman, Hall and Associates, 71% of health systems reported distribution delays; 58% surveyed reported raw product and sourcing availability disruptions.1
ECRI included supply chain disruptions in its annual Top 10 Patient Safety Concerns in 2021 and 2022. While supply chain challenges are anticipated to remain, nonacute care facility leaders can implement proactive strategies to achieve supply chain resilience and avoid disrupting or delaying necessary patient care.
Substituting Products: A Strategy That Works
Identifying substitute products in advance is one way to ensure a more flexible supply chain that anticipates and manages supply disruptions, backorders, and product recalls. Organizations should have a comprehensive supply chain strategy that addresses these key questions:
- Which substitute products could be used instead of current products?
- What are the best substitute suppliers and products to use?
- What lower- or equivalent-cost products, with equal or better effectiveness, would better serve the facility?
If leaders do not have a robust system that addresses these questions, their supply chain could be at risk. Here are three recommendations for selecting safe substitutes.
1. Assess Inventory to Pinpoint Opportunities for Standardization
Identifying clinically safe, acceptable substitutions for existing inventory is not only critical for navigating backorders, but can also be an effective tool in vendor negotiations. For instance, thousands of procedure kits are currently available. Finding one standard kit that meets a clinical care team’s needs and purchasing many kits can bolster negotiations with vendors, potentially resulting in better prices and savings opportunities for the organization. To minimize risks when standardizing to one vendor, keep relationships with an appropriate number of vendors and distributors and ensure that staff are using consistent products. Leaders should maintain a set inventory of substitute products that can be ordered when a supply disruption occurs or is anticipated.
To build organizational alignment, it is important to include clinicians, nurses, supply chain leaders, and other healthcare personnel in the standardization decision-making process. Successful standardization begins by having quality data. With strong data, actionable analytics, and visibility into all aspects of the supply chain, organizations can make better decisions, improve operational efficiency, and improve the bottom line. Also, standardization can help minimize variation in the quality of products and patient care, maximize contract compliance, reduce the number of stock-keeping units, and save money and time.
2. Establish Internal Protocols to Navigate Backorders in Advance of Disruption
Over the last three years, healthcare organizations have had to adapt quicky to address challenges in an ever-changing environment. Supply-chain management has never been more important to healthcare providers. Building preparedness plans to ensure that an available stock of critical supplies has become even more critical. The plan should include testing supply availability in emergency preparedness plans and drills. Leaders should evaluate current inventory planning, materials management, and procurement processes and work closely with vendors and other supply- chain partners to develop processes to anticipate and prevent backorders and recalls.
3. Build a Plan for Assessment and SelectionMany healthcare facilities encounter a common hurdle: the inability to objectively compare products based on vendor data and usage. When considering substitute products, organizations must carefully compare existing products with potential substitutes and collect independent, trustworthy data based on evidence.
New products are released into the market regularly with purported promises of clinical superiority over existing products, and clinician preference can also influence inventory decisions. Building a standard evaluation process that includes key performance indicators (KPIs) can help ensure that substitute products being considered are the right fit and meet product specification requirements and clinical, financial, and outcome expectations. KPIs are criteria used to evaluate critical areas of clinical and support functions that influence patient outcomes. With clear visibility to the KPIs used in compared products, purchasing managers and clinicians can collaborate to ensure they are making the best decisions on cost-effective, quality patient care.
To learn more about how ECRI can help strengthen your supply chain, download ECRI’s free white paper and reach out to an ECRI expert for a consultation.
1https://www.kaufmanhall.com/sites/default/files/2022-10/2022-State-Healthcare-Performance-Improvement.pdf
